
Living with both depression and anxiety can feel like being pulled in opposite directions, exhaustion and restlessness, numbness and overwhelm, all at once. If you're experiencing these overlapping conditions, you're not alone. Research shows that nearly 60% of people with anxiety also experience symptoms of depression. The good news is that therapy for depression and anxiety has evolved significantly, offering multiple evidence-based approaches that address both conditions at the same time.
At Reflective Therapy Center, we understand that finding the right treatment can feel overwhelming when you're already struggling. Our therapists work with clients every day who are navigating this exact challenge, matching specific therapeutic techniques to each person's unique situation rather than relying on a one-size-fits-all method.
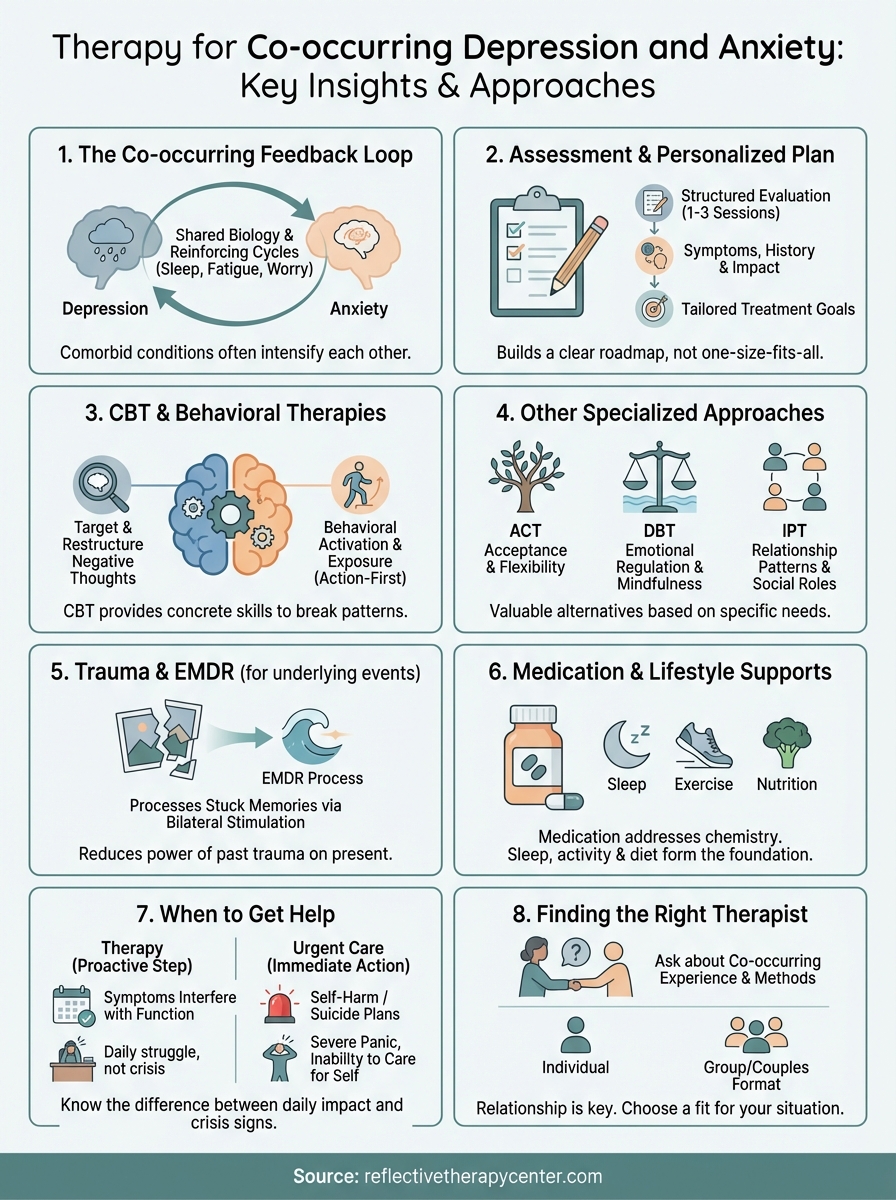
This guide walks you through the different types of therapy available for co-occurring depression and anxiety, what the treatment process actually looks like, and how to find clinical support that fits your needs. Whether you're considering individual sessions, exploring options like CBT or EMDR, or simply trying to understand what's out there, you'll leave with a clearer picture of your next steps toward feeling more like yourself.
Why depression and anxiety often show up together
Depression and anxiety aren't just coincidental companions. They share biological roots in your brain's chemistry and create a feedback loop that makes each condition harder to manage on its own. When you experience both, you're dealing with what clinicians call comorbid conditions, meaning they coexist and often intensify each other's symptoms. Understanding this connection helps you recognize why therapy for depression and anxiety needs to address both simultaneously rather than treating them as separate problems.

Shared brain chemistry and neural pathways
Your brain uses the same chemical messengers to regulate both mood and anxiety responses. Serotonin, dopamine, and norepinephrine all play roles in how you experience pleasure, motivation, worry, and fear. When these neurotransmitters function below optimal levels, you may notice low mood and heightened nervousness appearing together. Research shows that the amygdala, your brain's fear center, becomes overactive in both conditions, while the prefrontal cortex, which helps regulate emotions, shows reduced activity.
The neural circuits that process threats and rewards overlap significantly. If you've experienced chronic stress or trauma, these pathways can become sensitized, making you more vulnerable to developing both conditions. Your brain essentially learns to stay in a state of alert while simultaneously struggling to find pleasure or motivation in daily activities.
How symptoms overlap and reinforce each other
You might recognize the exhausting cycle: anxiety keeps you awake at night, leading to fatigue that worsens depressive symptoms the next day. That fatigue makes it harder to manage anxious thoughts, which then disrupts your sleep again. This pattern creates what therapists call a maintaining cycle, where each condition feeds the other.
When depression drains your energy and anxiety fills your mind with racing thoughts, you're caught between wanting to do nothing and feeling unable to rest.
Physical symptoms blur the lines even further. Restlessness, difficulty concentrating, and changes in appetite appear in both conditions, making it challenging to identify which issue you're addressing at any given moment. Many people describe feeling simultaneously wired and tired, unable to relax yet lacking the energy to engage with life. Your body stays in a state of tension while your motivation to address that tension remains low.
Common triggers that activate both conditions
Certain life circumstances trigger both conditions at once. Major life transitions like job loss, relationship changes, or health diagnoses create uncertainty that fuels anxiety while also threatening your sense of identity and purpose, which deepens depression. You're simultaneously worried about what might happen and feeling hopeless about your ability to handle it.
Chronic stress serves as another shared trigger. When you face ongoing demands without adequate recovery time, your nervous system stays activated, producing anxiety symptoms. Meanwhile, that same prolonged stress depletes your physical and emotional resources, creating the fatigue and disconnection characteristic of depression. Your body and mind become stuck in survival mode with no clear path to safety or relief.
Social isolation intensifies both conditions through different mechanisms. Loneliness activates threat responses in your brain similar to physical danger, generating anxiety. At the same time, reduced social contact removes the support and positive experiences that typically buffer against depression. You may withdraw because you feel anxious in social situations, then feel more depressed because of that isolation, creating another reinforcing loop that becomes increasingly difficult to break without professional intervention.
Understanding these connections explains why effective treatment addresses the underlying patterns that sustain both conditions rather than simply managing symptoms of each separately. Your therapist will recognize how these issues interact in your specific situation and design interventions that interrupt the cycles keeping you stuck.
When therapy can help and when to get urgent care
Knowing when to start therapy versus when you need immediate intervention can feel confusing when you're in the middle of overwhelming symptoms. Therapy for depression and anxiety works best as a proactive step, not just a crisis response, but certain situations require urgent medical attention before you begin regular treatment. Understanding this distinction helps you access the right level of care at the right time, protecting your safety while also getting the support that addresses your underlying conditions.

Signs that therapy is appropriate now
You should consider starting therapy when symptoms interfere with your daily functioning even if you're not in immediate danger. If you notice yourself canceling plans repeatedly due to anxiety, struggling to complete work tasks because of low motivation, or experiencing persistent worry that won't quiet down, these patterns signal that professional support can help before things escalate. Your sleep quality has shifted noticeably, you've withdrawn from relationships that used to matter, or you feel trapped in negative thought cycles that you can't break on your own.
Physical symptoms like tension headaches, digestive issues, or unexplained fatigue that your doctor has ruled out medical causes for often indicate anxiety and depression requiring therapeutic attention. You're functioning at work and home but notice you're operating on autopilot, feeling disconnected from experiences that used to bring satisfaction. These situations benefit from therapy's structured approach to changing thought patterns and building coping strategies, even when you're managing to get through each day.
Waiting until you're in crisis to seek help makes treatment harder, not because you've failed but because you're trying to build skills while your nervous system is overwhelmed.
Warning signs that require immediate help
Certain symptoms demand urgent medical care rather than scheduling a therapy appointment for next week. If you experience thoughts of harming yourself, detailed plans for suicide, or urges to act on those thoughts, you need to contact a crisis line immediately or go to your nearest emergency room. Active self-harm behaviors, inability to care for basic needs like eating or hygiene for several days, or complete loss of touch with reality through severe dissociation or psychotic symptoms all require crisis intervention before beginning outpatient therapy.
Severe panic attacks that leave you unable to function, especially if they're increasing in frequency or intensity, may require medication management and stabilization before traditional therapy can be effective. You might notice extreme mood swings, impulsive behaviors that put you at risk, or substance use that's escalated beyond your control. These situations call for immediate evaluation at an urgent care center or psychiatric emergency service, where professionals can assess whether you need intensive treatment like partial hospitalization before transitioning to regular therapy sessions.
What happens in an evaluation and treatment plan
Walking into your first therapy appointment, you'll participate in a structured assessment process that helps your therapist understand your specific combination of depression and anxiety symptoms. This evaluation creates the foundation for your treatment plan, giving both you and your provider a clear picture of where you're starting and what you're working toward. The process typically unfolds over one to three sessions, depending on the complexity of your situation and the thoroughness of your therapist's approach.
Your first assessment session
Your therapist will ask detailed questions about your current symptoms, their duration, and their impact on different areas of your life. You'll discuss when you first noticed these feelings, what situations make them better or worse, and how they affect your work, relationships, and daily routines. Expect questions about your sleep patterns, appetite changes, energy levels, and any physical symptoms you experience alongside emotional distress. Your provider will also explore your personal history, including previous mental health treatment, family patterns of depression or anxiety, and significant life events that may contribute to your current state.
This session includes screening tools and questionnaires that measure symptom severity using standardized scales. These assessments give your therapist objective data about where you fall on the spectrum of depression and anxiety, helping them determine the appropriate level of care. You'll answer questions honestly about your thoughts, including any concerning patterns that require immediate attention before beginning regular therapy for depression and anxiety.
Your therapist uses this information not to judge you but to create a roadmap that addresses your specific needs rather than applying generic strategies.
Creating your personalized treatment plan
After gathering comprehensive information, your therapist will develop a treatment plan tailored to your situation. This plan outlines specific goals you want to achieve, the therapeutic approaches that fit your needs, and a timeline for reassessing your progress. Your provider will explain which techniques they recommend and why, whether that's cognitive behavioral strategies, trauma processing, or interpersonal skills development. You'll discuss the frequency of sessions, typically starting weekly for moderate to severe symptoms, and what you can expect between appointments.
Treatment plans remain flexible documents that evolve as you progress. Your therapist will identify concrete targets like reducing panic attacks from daily to weekly, improving your ability to leave the house for social activities, or developing skills to interrupt rumination cycles. These specific markers help both of you track whether the approach is working or needs adjustment based on your response to treatment.
CBT and behavioral therapies for mood and anxiety
Cognitive behavioral therapy (CBT) stands as the most researched and validated approach for treating both depression and anxiety simultaneously. Your therapist uses CBT to help you identify the specific thought patterns and behaviors that maintain your symptoms, then systematically replaces them with more adaptive responses. Unlike approaches that focus solely on feelings, CBT gives you concrete techniques you can practice between sessions, making it particularly effective for people who want actionable strategies. Research consistently shows that CBT produces lasting changes because you learn skills that continue working long after treatment ends.

How CBT targets thought patterns in both conditions
Your therapist will help you recognize automatic negative thoughts that surface throughout your day, the reflexive judgments and predictions that fuel both depression and anxiety. For depression, these often take the form of harsh self-criticism or hopeless predictions about your future. With anxiety, you'll notice catastrophic thinking patterns where your mind jumps to worst-case scenarios before considering more realistic outcomes. CBT teaches you to catch these thoughts as they happen rather than accepting them as facts.
Once you identify these patterns, you'll learn cognitive restructuring techniques that challenge distorted thinking. Your therapist might ask you to examine the evidence supporting and contradicting your anxious predictions or depressive conclusions. You'll practice generating alternative explanations for situations that typically trigger negative thoughts, building flexibility in how you interpret events. This process doesn't involve forcing positive thinking but rather developing a more balanced and realistic perspective that reduces the intensity of your emotional responses.
When you change how you interpret situations, you change how your body responds to them, breaking the cycle that keeps both anxiety and depression active.
Behavioral activation and exposure work
Behavioral activation addresses the withdrawal and inactivity that depression creates by helping you reengage with activities that provide satisfaction or accomplishment. Your therapist will work with you to identify specific behaviors you've stopped doing, then create a structured plan to gradually reintroduce them. This might include scheduling time with friends, returning to hobbies, or completing small tasks that give you a sense of competence. The technique works because action often precedes motivation rather than following it.
For anxiety, CBT incorporates exposure therapy that gradually faces feared situations in a controlled way. You'll create a hierarchy of anxiety-provoking scenarios with your therapist, starting with situations that cause mild discomfort and progressing to more challenging ones as you build confidence. This systematic approach to therapy for depression and anxiety teaches your nervous system that these situations are manageable, reducing avoidance behaviors that maintain both conditions over time.
Other therapy options like ACT, DBT, and IPT
Beyond CBT, several specialized therapeutic approaches offer effective treatment for co-occurring depression and anxiety by targeting different aspects of your experience. These methods recognize that people respond differently to various techniques, making them valuable alternatives or complements to cognitive behavioral strategies. Your therapist might recommend one of these approaches based on your specific symptom patterns, personal preferences, or previous treatment responses. Each therapy brings unique tools that address the ways depression and anxiety show up in your life.
Acceptance and Commitment Therapy (ACT) for psychological flexibility
ACT teaches you to change your relationship with difficult thoughts and feelings rather than trying to eliminate them. Instead of fighting against anxious or depressive thoughts, you'll learn to notice them without letting them control your actions. This approach focuses on psychological flexibility, helping you move toward what matters to you even when uncomfortable emotions arise. Your therapist will guide you through exercises that build mindfulness skills and clarify your personal values.
The therapy emphasizes committed action aligned with your values rather than feeling good as the primary goal. You'll identify what gives your life meaning, whether that's relationships, creative pursuits, or contribution to your community, then take steps in those directions regardless of whether anxiety or depression show up. This framework proves particularly helpful when you feel stuck between anxious avoidance and depressive withdrawal, giving you a different metric for success beyond symptom reduction.
Dialectical Behavior Therapy (DBT) for emotional regulation
DBT combines cognitive behavioral techniques with mindfulness and acceptance strategies, originally developed for intense emotional experiences. Your therapist will teach you four core skill sets: mindfulness for staying present, distress tolerance for managing crises without making things worse, emotion regulation for reducing vulnerability to mood swings, and interpersonal effectiveness for maintaining relationships while respecting your needs. These skills address the emotional intensity that often accompanies severe anxiety and depression.
When you learn to tolerate distress without reacting impulsively, you break the patterns that keep both conditions active.
This approach works especially well if you experience rapid emotional shifts or engage in behaviors that provide temporary relief but worsen your situation long-term. Through structured skills training and individual sessions, you'll build capacity to handle difficult situations more effectively, reducing the frequency and intensity of both anxious and depressive episodes.
Interpersonal Therapy (IPT) for relationship patterns
IPT focuses on how your relationships and social roles contribute to depression and anxiety. Your therapist will help you identify specific interpersonal issues, whether that's unresolved grief, role transitions like becoming a parent or losing a job, relationship conflicts, or social isolation. The approach recognizes that improving your connections with others often reduces symptoms of both conditions by addressing the loneliness and conflict that maintain them.
Treatment concentrates on developing communication skills and resolving relationship problems in the present rather than exploring childhood experiences. You'll work on expressing your needs clearly, setting boundaries with others, and building a support network that sustains your mental health. IPT proves particularly effective for therapy for depression and anxiety when your symptoms connect directly to relationship stress or life transitions that have disrupted your social connections.
Trauma-focused therapy and EMDR for related trauma
Your depression and anxiety may stem from past traumatic experiences that continue affecting how your brain processes current situations. Trauma-focused therapies address these underlying events directly rather than only managing the symptoms they produce. When you've experienced abuse, accidents, violence, or other overwhelming events, traditional talk therapy might not access the way your nervous system stored those memories. Specialized approaches work with how your brain holds traumatic material, helping you process what happened so it stops triggering present-day distress.

When trauma underlies your depression and anxiety
You might recognize trauma's role if you experience intrusive memories, flashbacks, or nightmares alongside your depressive and anxious symptoms. Your nervous system may react to current situations as if past dangers are happening now, creating anxiety responses that feel out of proportion to what's actually occurring. Depression often develops when trauma leaves you feeling powerless, disconnected from others, or convinced the world is unsafe. Many people don't initially connect their mood symptoms to earlier experiences because the trauma occurred years ago or seemed "not bad enough" to matter.
Your body holds trauma even when your conscious mind tries to forget it. Physical tension, hypervigilance, or sudden panic in response to seemingly random triggers all suggest unprocessed traumatic material. Therapy for depression and anxiety becomes more effective when it addresses these foundational experiences rather than treating only the surface symptoms they generate.
How EMDR processes traumatic memories
Eye Movement Desensitization and Reprocessing (EMDR) helps your brain reprocess stuck traumatic memories through bilateral stimulation while you recall distressing events. Your therapist will guide your eyes to follow their hand movements or use tapping or audio tones that alternate between your left and right sides. This process activates the same neural mechanisms your brain uses during REM sleep to integrate experiences, allowing traumatic memories to move from their frozen state into regular memory storage.
EMDR doesn't erase what happened but changes how your brain and body respond to those memories, reducing their power over your present life.
During sessions, you'll identify specific traumatic memories contributing to your current symptoms, along with the negative beliefs about yourself those events created. Your therapist will help you process these memories in a structured way that feels manageable rather than retraumatizing. Most people notice reduced emotional intensity around traumatic memories within several sessions, though complex trauma requires longer treatment.
What happens in trauma processing sessions
Your therapist will prepare you with grounding techniques and coping skills before beginning memory processing work. You'll learn how to regulate your nervous system and return to the present if the work becomes overwhelming. This preparation phase ensures you have the resources to handle difficult material safely, building a foundation that supports the deeper processing work ahead.
Treatment progresses through eight structured phases that move from history gathering through memory reprocessing to integrating new perspectives about yourself and your future. Your therapist will check in regularly about your capacity to continue, adjusting the pace based on how you're responding to the work.
Medication, combined care, and lifestyle supports
Therapy for depression and anxiety works most effectively when it's part of a comprehensive approach that addresses multiple factors affecting your mental health. While psychotherapy provides essential skills and insight, many people benefit from medication, lifestyle modifications, or a combination of treatments working together. Your symptoms, severity, and personal preferences all influence which combination makes sense for you. Understanding how these elements support each other helps you make informed decisions about your treatment plan.
When medication works alongside therapy
Your therapist or psychiatrist might recommend antidepressant or anti-anxiety medication when symptoms interfere significantly with your ability to participate in therapy or function daily. Medications like SSRIs (selective serotonin reuptake inhibitors) or SNRIs (serotonin-norepinephrine reuptake inhibitors) address the brain chemistry imbalances underlying both conditions, often making it easier to engage with therapeutic techniques. You'll typically notice medication effects within two to six weeks, though finding the right medication and dosage sometimes requires adjustments.
Combined treatment proves particularly effective for moderate to severe depression and anxiety. Research shows that people receiving both therapy and medication often experience faster improvement and better long-term outcomes than those using either approach alone. Your therapist can't prescribe medication but will coordinate with your prescriber to ensure your treatment plan addresses all aspects of your recovery. This integrated approach allows medication to reduce symptom intensity while therapy builds the skills you need to maintain progress.
Building lifestyle foundations that support treatment
Sleep quality directly affects both your mood regulation and anxiety levels, making it a primary target alongside formal treatment. Your therapist will help you establish consistent sleep schedules and address habits that disrupt rest, recognizing that poor sleep perpetuates the cycle of both conditions. Regular physical activity serves as another powerful support, with research showing that exercise produces changes in brain chemistry similar to antidepressants while reducing physical tension associated with anxiety.
Nutrition impacts your mental health through multiple pathways, from blood sugar stability to gut bacteria that influence neurotransmitter production. Your treatment plan might include working with a nutritionist to address deficiencies or patterns that worsen symptoms. Social connections and meaningful activities provide structure and positive experiences that counter isolation and hopelessness, making them essential components rather than optional additions to your recovery process.
Lifestyle changes don't replace professional treatment, but they create the foundation that allows therapy and medication to work more effectively.
How to choose the right therapist and format
Finding the right therapist requires more than checking insurance coverage or picking the first available appointment. You're looking for someone who understands how depression and anxiety interact in your specific situation and uses approaches that fit your needs. The therapeutic relationship itself predicts treatment success more than any particular technique, making it worth investing time to find a provider you connect with. You'll know you've found a good match when you feel heard without judgment and notice concrete progress within the first few sessions of therapy for depression and anxiety.
Questions to ask potential therapists
Start by confirming their experience treating co-occurring depression and anxiety rather than just one condition. Ask which therapeutic approaches they use most often and how they decide which techniques to apply. You want to understand their treatment philosophy and whether they take a flexible approach or strictly follow one method. Find out how they measure progress, what they expect from you between sessions, and how they handle situations when treatment isn't working as planned.
Your practical concerns matter equally to clinical expertise. Clarify their availability for emergencies, policies around canceled appointments, and typical treatment duration for someone with your symptom severity. Ask whether they coordinate with other providers if you're taking medication or need additional services. Their answers reveal how they structure care and whether their approach aligns with what you need to feel supported throughout treatment.
The right therapist will answer your questions directly and help you understand what to expect rather than making you feel awkward for asking.
Comparing individual, couples, and group formats
Individual therapy provides personalized attention where your therapist tailors every session to your current needs and progress. This format works best when your symptoms primarily affect your personal functioning or when you need privacy to address sensitive material. You'll build specific skills at your own pace without worrying about others' progress or concerns taking session time.
Couples therapy addresses how depression and anxiety affect your relationship and how relationship patterns might worsen your symptoms. Your therapist helps both partners understand these conditions and develop strategies that support your mental health while strengthening your connection. Group therapy offers peer support and reduces isolation by connecting you with others facing similar challenges, though you'll receive less individualized attention than in private sessions. Many people combine formats, starting with individual work then adding group or couples sessions as they progress.
Where to go from here
Starting therapy for depression and anxiety represents a significant step toward feeling better, not a sign of weakness or failure. You now understand the treatment options available, from cognitive behavioral approaches to trauma-focused work, and how these therapies address the ways both conditions interact. Your next move involves taking action rather than waiting for the perfect moment or complete certainty about which approach fits best.
Contact providers who specialize in treating co-occurring conditions and schedule initial consultations with two or three therapists. You'll discover through those conversations whether their approach and communication style match what you need. If you're in the area and looking for experienced clinicians who treat both depression and anxiety, Reflective Therapy Center offers comprehensive evaluations and evidence-based treatment that addresses your specific situation. Your mental health deserves the same attention you'd give any other aspect of your wellbeing, and the right support makes recovery possible.